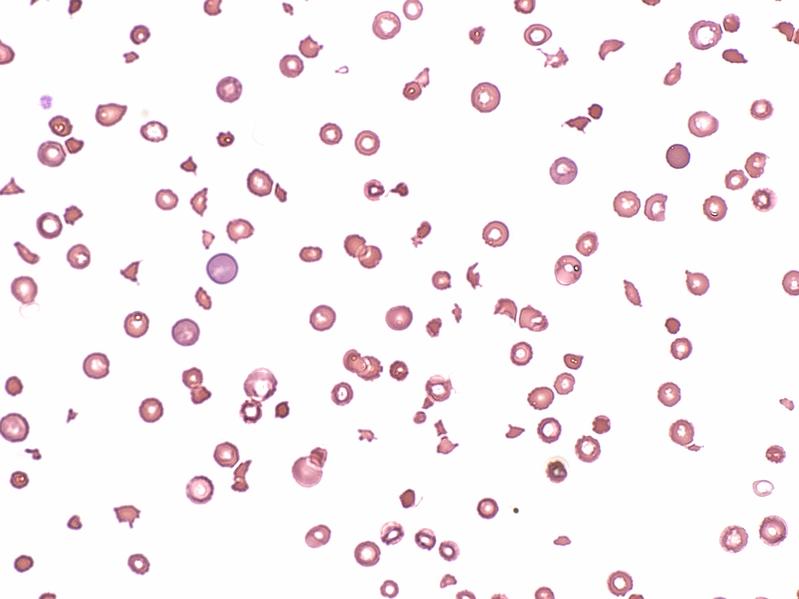
Effective treatment for rare blood disorder
Anyone who survives an acute episode of the rare blood disorder TTP is often left with long-term consequences, especially neurological damage. An international study, with the participation of the Department of Hematology of Bern University Hospital, was now able to verify the effectiveness of a new innovative treatment.
The life-threatening blood disorder thrombotic thrombocytopenic purpura (TTP) is rare (2-3 people out of every million per year) and affects mainly young, otherwise healthy people – women more frequently than men. TTP will lead to death if not treated within a few days.
In healthy individuals, the protein scissor ADAMTS13 cleaves ultra large von Willebrand factor (VWF) multimers. Smaller VWF multimers are less sticky, do not bind platelets spontaneously and thus formation of blood clots in blood vessels is prevented. In TTP, ADAMTS13 is lacking due to circulating autoantibodies. In the absence of VWF size regulation, platelets are consumed in VWF-platelet clots, that occlude the microcirculation. Blood circulation to end organs is decreased, resulting in heart attack, stroke and kidney failure. Hence TTP is also been refered to as “clumping plague”.
So far, standard treatment of acute episodes of TTP consists of a daily plasma exchange (to remove autoantibodies and replenish ADAMTS13) in combination with immunsuppressive drugs (to inhibit autoantibody formation). Nevertheless, 10 - 20 percent of patients die during an acute episode. In addition, more than half of the survivors have permanent organ damage and dysfunction, particularly in the form of neurological deficits, and frequently experience relapses.
Rapid control of the disorder with lower rate of relapses
A major international study, with the participation of the Department of Hematology of Bern University Hospital, was published on January 9, 2019, in the New England Journal of Medicine (NEJM). The study was able to confirm the effectiveness of an innovative TTP treatment. The studied anti-VWF nanobody, caplacizumab, was shown to effectively prevent VWF-platelet clumping and thus protect the end organs from further depriviation of blood circulation.
145 TTP patients partcipated in this randomized Phase III study, 72 received the nanobody during the plasma exchange treatment and for 30 days thereafter, 73 received a placebo for the same period of time. In 75 percent of patients who received the study drug, the acute phase of TTP ended after 2.95 days, compared to 4.5 days with the conventional treatment. Furthermore, the patients required fewer plasma exchange sessions (median 5 vs. 7), and could be discharged earlier. The side-effects were comparable in both study arms, although mild bleeding symptoms occurred more frequently with the new compound (65% compared to 48% with placebo). The study was able to confirm the promising data of the Phase II study, in which the Bern-based Hematology Department had also participated.
Long-term research topic at the Bern University Hospital and Bern University
The Department of Hematology at the Bern University Hospital and Bern University (Hematology Research Group, Department of BioMedical Research) have been researching TTP and ADAMTS13 since the mid-1990s. This resarch was initiated by Prof. em. Dr. phil nat. Miha Furlan and Prof. em. Dr. med. Bernhard Lämmle with the discovery of the von Willebrand factor-cleaving protease (now ADAMTS13), and the observation of its deficiency in TTP, and is currently headed by Prof. Dr. med. Johanna Kremer Hovinga. Since 2010 she has been involved in developing the new treatment approach for TTP, which will be available to all TTP patients in the future.
Wissenschaftlicher Ansprechpartner:
Prof. Dr. med. Johanna A. Kremer Hovinga Strebel, Senior Consulting Physician, Department of Hematology and Central Hematology Laboratory, Inselspital, Bern University Hospital, Johanna.Kremer@insel.ch
Originalpublikation:
DOI: 10.1056/NEJMoa1806311
Weitere Informationen:
https://www.nejm.org/doi/full/10.1056/NEJMoa1806311
Die semantisch ähnlichsten Pressemitteilungen im idw