Vaccinating against cancer? - A new class of vaccines developed
A vaccination as tumor therapy - with a vaccine individually created from a patient's tissue sample that " attaches" the body's own immune system to cancer cells: the basis for this long-term vision has now been achieved by a team of researchers from the MPI for Polymer Research and the University Medical Center Mainz, in particular from the Departments of Immunology and Dermatology. Their results were recently published in the journal ACS Nano.
"We have implemented a new class of vaccines that could form an efficient alternative to mRNA vaccines," says Prof. Dr. Lutz Nuhn, so far group leader in Tanja Weil's department at the MPI for Polymer Research and recently appointed as Professor of Macromolecular Chemistry at the Julius-Maximilians-University in Würzburg. This is important, for instance, for people in whose bodies the production of proteins is disturbed when they are vaccinated with mRNA vaccines - i.e. those that are sometimes used against corona - and for whom these vaccines therefore only have a limited effect.
The main reason, however, is that if Vaccines against cancer are to become the norm one day, various effective strategies must be explored to provide specific immune cells with essential key information.
Antigen plus immune activator - coupled to nanoparticles
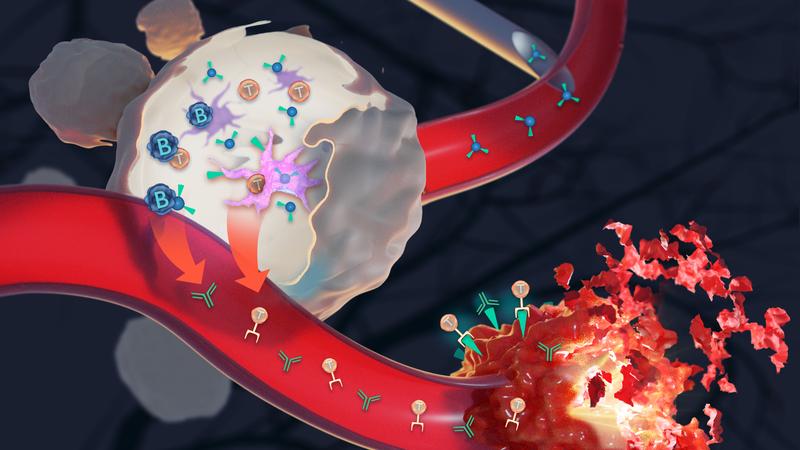
The novel vaccine class consists of two components: Firstly, the antigen, which is specific to the tumor cell and is to be recognized by the immune system as an "enemy", so to speak, and secondly, the immune activator - a "stinger" that shakes up the immune system.
As the immune activator, the researchers use the derivative of a chemical molecule that was discovered by Sunil A. David in the USA and is already being used successfully in the Indian corona vaccine Covaxin. By itself, this molecule is too active and potent and would cause violent inflammatory reactions throughout the body. Therefore, the research team attaches it to a carrier - more precisely, to polymer-based nanoparticles that have a gel-like consistency, are biodegradable and locally limit the effect of the immune activator. These nanoscale materials with diameters of less than 100 nanometers are about the size of viruses - the cells of the immune system therefore recognize them very well, eat them and in this way awaken from their dormant mode. The nanoparticles thus open up a direct pathway into the immune system. And: "By binding them to nanopolymers, we were able to throttle the immune response to the desired level," explains Nuhn.
Vaccine specifically kills tumor cells
For the vaccine to target the tumor, you need to know: What distinguishes tumor tissue from healthy tissue - in other words, which specific antigens are found on the cancer? This may well be patient-specific. "If a tumor is diagnosed in the early stages, a race against time begins to produce the patient-specific vaccine as quickly as possible," Nuhn explains.
To develop the new vaccine classes, the researchers first use a model antigen. They have generated various tumors that carry this model antigen - either on the surface or inside. Initial studies are promising; the T cells activated by the vaccine only kill tumor cells that carry the antigen on their surface or even inside. Healthy tissue, on the other hand, is not affected. "The polymer-based nanocarrier is a helpful toolbox to further evaluate antigen-specific vaccines and to develop further vaccine-based therapeutic concepts against cancer," Nuhn is convinced. One thing must be said, however: Several years of further research will be needed before such vaccines can cure patients of tumors. Nor will it be possible to combat all types of cancer with a vaccine.
Wissenschaftlicher Ansprechpartner:
Prof. Dr. Lutz Nuhn
T: +49 6131 379-311
lutz.nuhn@mpip-mainz.mpg.de
Originalpublikation:
Stickdorn, J.; Stein, L.; Arnold-Schild, D.; Hahlbrock, J.; Medina-Montano, C.; Bartneck, J.; Ziß, T.; Montermann, E.; Kappel, C.; Hobernik, D. et al.: Systemically Administered TLR7/8 Agonist and Antigen-Conjugated Nanogels Govern Immune Responses against Tumors. ACS Nano 16 (3), S. 4426 - 4443 (2022)
https://dx.doi.org/10.1021/acsnano.1c10709
Ähnliche Pressemitteilungen im idw