Hope for the treatment of people with severe burns
MHH researchers are developing an innovative drug to prevent the rejection of donor skin grafts.
When people suffer severe burns, there is not only a risk of infection in the wound. The high loss of fluid can also result in life-threatening circulatory shock. Therefore, the destroyed skin must be replaced as quickly as possible. Ideally, the wounds are treated with the patient's own skin from healthy parts of the body, so-called split-thickness skin grafts. However, the tissue is often insufficient to cover these skin defects. Furthermore, the removal of skin can lead to further complications. In such cases, surgeons use biological and synthetic skin substitutes to cover the wound, at least temporarily. However, so far it has not been possible to produce a full-fledged skin substitute that can be used anywhere and does not cause any rejection reactions. Professor Dr Peter M. Vogt, Director of the Department of Plastic, Aesthetic, Hand and Reconstructive Surgery at the Hannover Medical School (MHH), and his scientific team want to change this. Since 2019, the researchers have been working on modifying a transplant made from human donor skin in such a way that the unwanted immune reaction of burn victims is optimally kept in check after surgery. The project ‘Development of a US11 biopharmaceutical for the local suppression of the immune response after transplantation’ is funded by the VHV Foundation and will now receive follow-up funding of around 770,000 euros for a further three years.
Tricking the immune system
Our immune system only accepts our own body cells. Anything that is ‘allogenic’, i.e. foreign to the body, is attacked. This also applies to transplants such as tissue or donor organs. The immune cells orient themselves using the so-called MHC proteins on the cell surfaces. These are, so to speak, the cell's ID card and vary from person to person. The T cells of the immune defence use the MHC proteins to decide whether they need to intervene or not. In order to prevent a transplant of human donor skin from being rejected, the immune defence must be suppressed with medication. However, this inhibition has a significant disadvantage: pathogens have an easy time of it and severe infectious diseases can result. In their project, the researchers are trying to outwit the immune system without completely paralysing the body's defences.
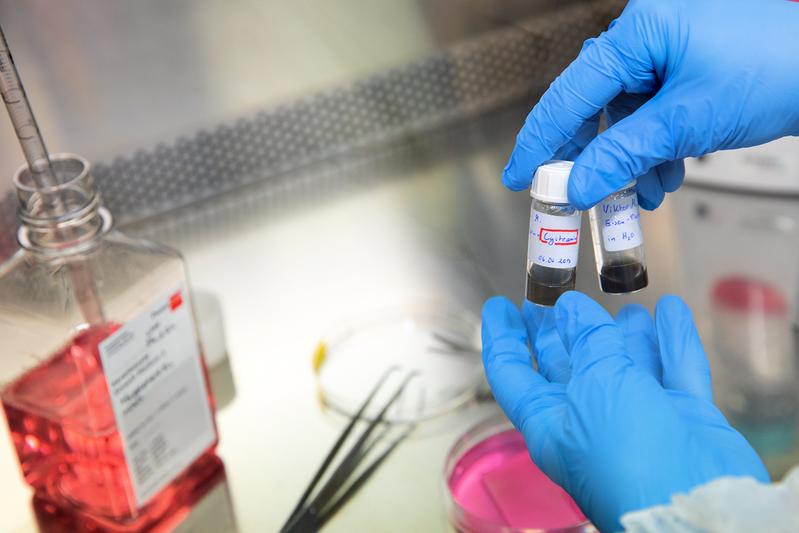
“We have modified tissue samples from our department's own skin bank so that the skin cells only display a certain group of MHC proteins called MHC-I in small quantities on their surface,” explains Dr Vesna Bucan, scientific director of the project. The tissue comes from donated “excess skin” that is left over from skin tightening operations in the clinic. “We process the living donor skin, test it microbiologically and virologically and store it in a special cryoprotective medium at minus 180°C for later transplantation,” says the human biologist. In an initial step, the researchers worked with viral vectors that, as gene taxis, transport the blueprint for a protein called US11 into the cells of the skin graft. The US11 protein produced inside the cell ensures that MHC-I is cut into several pieces and disposed of. “Since most MHC-I proteins no longer reach the cell surface, the immune system does not immediately recognise the cell as foreign and the immune response is significantly weaker,” notes Dr Bucan.
Safely packed into the target cell
In the next step, the research group wants to deliver US11 directly to the cell without the help of a gene taxi, in order to make the protein even more effective. To prevent it from breaking down prematurely on its way into the cell, it will be encapsulated in so-called niosomes. These are microscopically small spheres that can protectively envelop the active ingredient and improve its transport into the target cell. “This novel and effective form of administration has already been tested and approved for the coronavirus vaccine from BioNTech, for example,” explains Professor Vogt. The working group is receiving support from the Institute for Particle Technology at the Technical University of Braunschweig.
The next step is to use a mouse model to determine the dosage at which the drug is most effective and well tolerated. US11 is currently still being produced by bacteria. In the long term, the protein will be produced synthetically to ensure consistent quality and exclude bacterial contamination. If all goes well, the drug could be used in the future to suppress the rejection of transplants made from donor skin without affecting the entire immune system. “This would not only make the work of medical staff easier, but also significantly reduce the burden on patients,” emphasises the clinic director.
For further information, please contact Professor Dr Peter M. Vogt , vogt.peter@mh-hannover.de.
Die semantisch ähnlichsten Pressemitteilungen im idw